Pituitary tumours have an estimated prevalence of somewhere between 15-22.5%, with clinically relevant pituitary adenomas occurring in 1/1000 individuals worldwide.
The clinical manifestations of pituitary adenomas are extremely broad, with emerging data clearly defining the impact of hormonal and neurological sequelae of many tumours impacting quality of life and life expectancy.
Although many pituitary tumours do not need treatment there are others that require surgical removal. This is usually because they are growing and are causing compression of some important structures, or in other cases where the hormones being secreted can have significant medical and physiological effects.
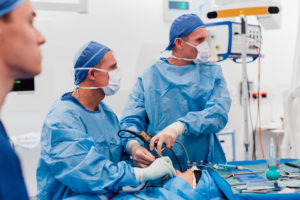
Endoscopic pituitary surgery, also called transsphenoidal endoscopic surgery, is the most common surgery used to remove pituitary tumors. The pituitary gland is located at the bottom of your brain and above the inside of your nose. It is responsible for regulating most of your body’s hormones.
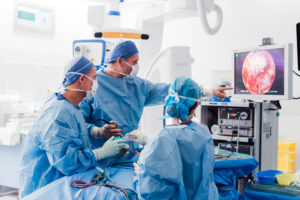
Endoscopic pituitary surgery is done with an endoscope. An endoscope is a thin, rigid tube that has a microscope, light, and camera built into it, and it’s usually inserted through the nose. The camera allows us to watch a magnified version of your tumour whilst we resect it from the surrounding structures.
St Vincent’s Hospital was the first Hospital in Australia to perform the removal of a pituitary tumour. This was performed by Sir Victor Horsely in 1952. Since that time St Vincent’s has been at the forefront of skull base surgery, where we are now striving to be a Centre of Excellence for Pituitary Tumour Management. We perform more pituitary surgeries than any other Hospital in NSW and have a dedicated team managing pituitary disorders.